Podcast: Play in new window | Download
Subscribe: RSS
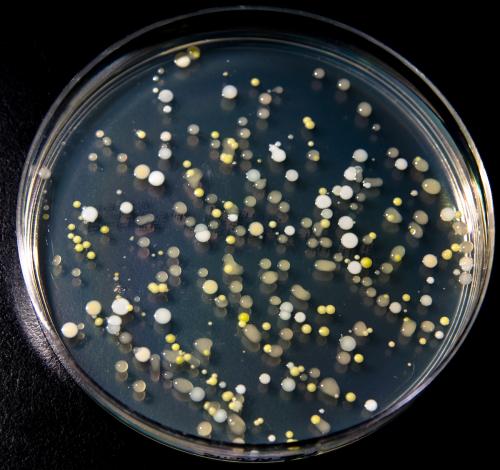
If global warming doesn’t get us, global sickening might; microbes like these are shrugging off modern medicine’s tools to control them. (Photo by Carlos de Paz/Flickr)
According to the World Health Organization, the planet is about to enter a post-antibiotic age in which minor infections kill us because the tools of modern medicine, which have been effective for a century and more, no longer work. The organization’s first global survey of drug-resistant disease found that in addition to antibiotic resistance by infectious bacteria — now well established everywhere in the world — resistance by viruses such as HIV, parasites including malaria and fungi is also spreading fast. All in all, says WHO, it is “a major threat to public health” whose “implications will be devastating.”
The report focused on antibiotic resistance among seven bacteria responsible for some of the most common serious infections. Its major findings:
- Resistance to the treatment of last resort for life-threatening infections caused by a common intestinal bacteria, Klebsiella pneumoniae–carbapenem antibiotics–has spread to all regions of the world. K. pneumoniae is a major cause of hospital-acquired infections such as pneumonia, bloodstream infections, infections in newborns and intensive-care unit patients. In some countries, because of resistance, carbapenem antibiotics would not work in more than half of people treated for K. pneumoniae infections.
- Resistance to one of the most widely used antibacterial medicines for the treatment of urinary tract infections caused by E. coli–fluoroquinolones–is very widespread. In the 1980s, when these drugs were first introduced, resistance was virtually zero. Today, there are countries in many parts of the world where this treatment is now ineffective in more than half of patients.
- Treatment failure to the last resort of treatment for gonorrhoea–third generation cephalosporins–has been confirmed in Austria, Australia, Canada, France, Japan, Norway, Slovenia, South Africa, Sweden and the United Kingdom. More than 1 million people are infected with gonorrhoea around the world every day.
- Antibiotic resistance causes people to be sick for longer and increases the risk of death. For example, people with MRSA (methicillin-resistant Staphylococcus aureus) are estimated to be 64% more likely to die than people with a non-resistant form of the infection. Resistance also increases the cost of health care with lengthier stays in hospital and more intensive care required.
The report makes only an offhand reference to the fact that the practices of industrial agriculture are at the root of the wildfire of antibiotic resistance that is now killing people worldwide. The massive administration of antibiotics to millions of animals in close confinement, not to cure them of infection but to prevent infection so as to maximize their growth and their owners’ profits, has provided optimum conditions for mutations to occur and spread to humans. [See Meat Industry: Have MRSA on Us; USDA Gets Bad News on Superbugs: Shoots Messenger; and Microbes Winning War on Terra]
It’s another example of how industrial methods for maximizing profits deliver the profits first, while risks engendered by the practices slowly accumulate until they emerge to extract their true terrible costs from innocent people.
Here’s a thought that was recently unthinkable but that is increasingly being expressed: If the only thing that will stop these people is a total crash of the system, then maybe we should think of a crash as more medicinal than destructive. You know, like chemotherapy.
I think I read somewhere that farmers use antibiotics not only to prevent infection but also because it makes the animals to grow faster and larger. Wonder what that has to do with the obesity epidemic…
We seem hell bent on destroying ourselves based on greed, convenience, or ignorance–call it what you will. People either don’t care (as in choose to ignore) or don’t know. I believe the latter is very prevalent and the direct consequence of the total decline of the media where instead of reporting the news it’s used as propaganda to push liberal and conservative agendas. Politicians, media types, industrialists, and activists of all stripes put so much spin on things that it’s dizzying to watch and hear. It makes it difficult for the average bloke to know the truth. It would be nice to see more widely reported stories like this one that show what is occurring, causes, and potential consequences. Yet, as you point out, no matter what the future holds things are eventually self correcting. Proving once again that excess of any kind usually leads to bad things happening. It’s just a matter of timing.
In case any readers missed it, I highly recommend watching the PBS-Frontline documentary Hunting the Nightmare Bacteria. A glimpse into yet another peril we will all be facing in the none-too-distant future. It should be clear to anyone paying attention that industrialized agriculture/livestock and the pharmaceutical companies are all about the motherf–kin’ money, all other “priorities” rescinded.